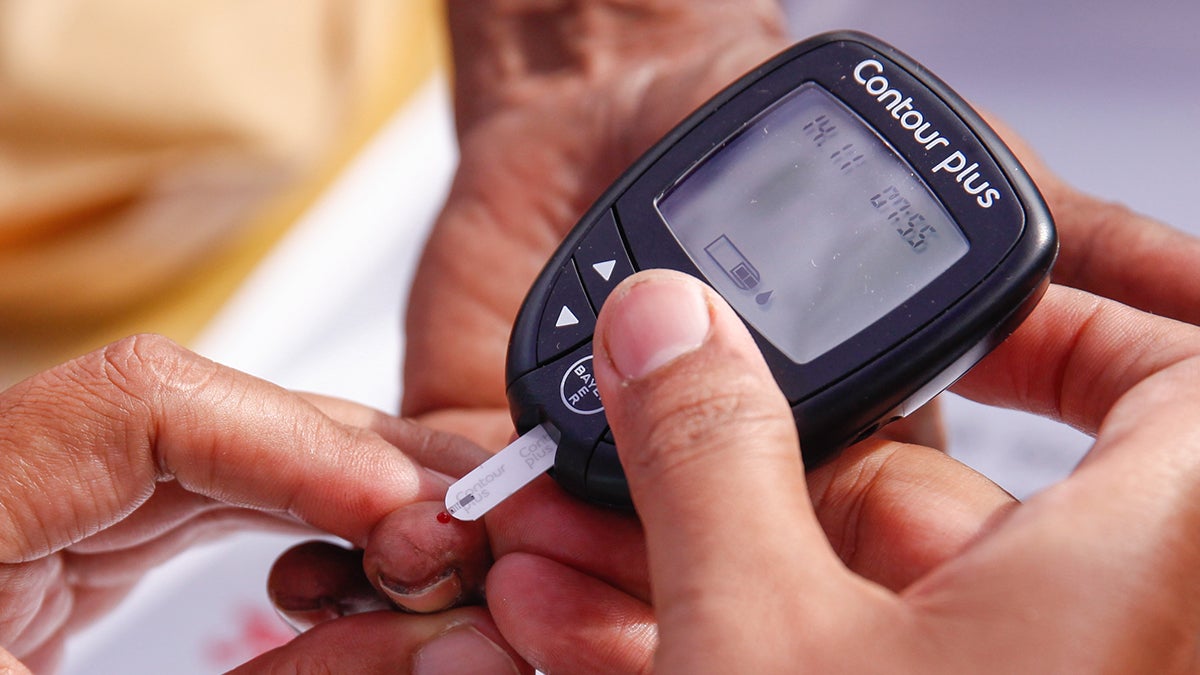
Endurance training can significantly impact diabetics
Why this matters
Endurance training can potentially hinder diabetics.
Gary Hall Jr., 10-time Olympic swimmer from 1996-2004 was at the peak of his career when he found out he had Type 1 diabetes.
At the time of his diagnosis he was told by doctors that his swimming career was over.
Like any Olympic-level athlete, Hall trained up to eight hours a day and ignored the symptoms he was having.
Hall explained his symptoms to Men’s Journal. He said he had blurry vision, extreme thirst, ate PowerBars to boost his blood sugar and burned an excessive amount of calories through running, weightlifting and boxing.
“The doctors said exercise was good in moderation, but not at the level I was at,” Hall said.
While Hall is only one example research has shown that endurance training can hinder diabetics if not properly monitored.
The Centers for Disease Control and Prevention’s National Diabetes Statistics Report in 2015 estimated 30.3 million people in the United States had Type 1 or Type 2 diabetes.
In Type 1 diabetes, which is more common in early childhood — and unpreventable — the immune system confuses healthy insulin cells and harmful invaders like bacteria and viruses, so the body destroys the insulin produced in the pancreas. Type 1 diabetes can be passed down genetically or develop at any point in a person’s life.
In Type 2 diabetes, the more common — and preventable — type, the body either does not respond to insulin or make enough insulin. While this type of the disease can develop at any age, it is more common in those who are 45 or older, overweight or obese, physically inactive or pregnant. While type 2 diabetes typically affects people of the aforementioned demographics, it can also be found in endurance athletes.
The German Sport University of Cologne conducted a study last year on whether “Endurance training (3 times per week for 3 months, moderate intensity) alters YKL40, PERM1 and HSP70 (protein levels) skeletal muscle protein contents in men with type 2 diabetes mellitus.”
In the study the men were separated into three groups T1 (6 weeks pre-training), T2 (1 week pre-training) and T3 (3-4 days post-training). Afterward muscle biopsies were taken by selectively imaging antigens in cells of a tissue or immunohistochemistry.
The results showed a significant upregulation following endurance training in all three protein levels.
The proteins HSP70 showed a “fiber type-specific distribution with increased protein contents” in those six weeks pre-training.
HSP70 or also known as ‘heat-shock protein’ are the main component of cell’s machinery. They produce ‘Protein Folding’ a process that gives proteins their 3-dimensional structure and protects cells from stress.
Those T3 (3-4 days post-training) showed a “significant change in the fiber type distribution with an increase in type I fibers and a decrease in type II fibers.”
However, when it came to T1 and T2 (6 weeks pre-training and 1 week pre-training) there was no significant differences or fiber type distribution for all protein levels (YKL40, PERM1, HSP70).
So with the increased training of all three protein levels the study found that it could help manage Type 2 diabetes and even reduce the risk of future complications.
Emma Willingham, Master of Science candidate in Nutrition, Healthspan, and Longevity at the University of Southern California, conducted a review on “The Management and Care of the Type 1 Diabetic Athlete” and found the “most important goal is to keep blood glucose levels at or as close to normal levels as possible without causing hypoglycemia” which requires the maintenance of a delicate balance between hypoglycemia, euglycemia and hyperglycemia.
Willingham first noted that finding a balance among them can be significantly more difficult to achieve in diabetic athletes due to the high demands of physical activity and competition.
As each athlete is different with a variety of factors like type, duration and intensity of exercise should be taken into consideration.
So extra care must be taken because with moderate intensity exercise a lowering effect of blood glucose increases the risk of developing an episode of hypoglycemia.
Without the proper balance, athletes can risk the result of “overinsulinization both during and after exercise,” said Willingham.
“The rate at which the body absorbs subcutaneously injected insulin increases with exercise due to an increase in body temperature and in subcutaneous muscle blood flow. Hypoglycemia can also result from an impaired release of counter regulatory hormones caused by a previous bout of exercise or a previous hypoglycemic episode,” said Willingham.
As a result, Willingham said professionals working with Type 1 diabetic athletes should advise the athlete to reduce their insulin dosage by 50-90 percent prior to activity. Or eating a low glycemic index pre-exercise meal is a good recommendation to help improve performance.
Additionally, with overinsulinization another risk factor that can occur is the psychological stress athletes can experience during a hypoglycemic episode.
According to Willingham, the psychological stress associated with competition frequently associated with increases in blood glucose levels before competition also causes an increase in counter regulatory hormone levels.
“Injury is also associated with increases in the secretion of these stress hormones and can also cause an increase in blood glucose levels — an exaggerated hyperglycemic response in people with Type 1 diabetes,” wrote Willingham.
Willingham explained that when caring for an athlete with Type 1 diabetes, the most important consideration is managing blood glucose levels, with particular attention to hyperglycemia. That is because the greater number and frequency of long-term complications from diabetes can be traced to hyperglycemia rather than hypoglycemia.
“For example, Type 1 diabetics should be screened annually for cardiovascular disease, retinopathy, nephropathy, neuropathy, and a foot exam to check sensory function and ankle reflexes,” wrote Willingham.
Willingham concluded if not properly monitored an athlete’s performance can deteriorate and “experience detrimental internal health effects.”
Cleveland Clinic explains that when an athlete’s blood sugar is not within a safe, normal level athletes are not allowed to exercise.
According to the Cleveland Clinic symptoms of low blood sugar (hypoglycemia) include body tremors, weakness, confusion, slurred speech and eventually coma. Symptoms of high blood sugar (hyperglycemia) include nausea, labored breathing, mental confusion or unconsciousness.
“Exercise some-times has the same effect on blood sugar as insulin and is most likely to lower your athlete’s blood sugar even more. Exercise is also not recommended with high blood sugar when ketones (determined through a urine test) are present,” according to Cleveland Clinic.
Martin B. Draznin, M.D., director of the Pediatric Endocrine Specialty Clinics at Michigan State University said in Men’s Journal, “Exercise has always been encouraged for diabetics because it can help to transport glucose into cells, reducing blood-sugar buildup. However, there are certain activities in which blood-glucose imbalances could lead to inattention and result in serious injury.”
Some of the activities include, “scuba diving, rock climbing, mountaineering — anything where you are really out on the edge and don’t have a lot of backup,” Draznin said.
For Hall, during his peak training he gave himself eight insulin shots daily, double the daily dosage for the average person.
Hall said with that much insulin, his body constantly craved carbohydrates for fuel.
“Basically, you have to have an idea of what every food you consume is going to do to you, and how your body is going to react to it. In a lot of ways, you have to be your own doctor,” said Hall.
“If you eat right, you should be able to cut down the amount of insulin you need,” said Sheri Colberg-Ochs, Ph.D., assistant professor of exercise science at Old Dominion University. “Adding fiber is usually recommended, as is substituting low-fat milk for whole milk and replacing saturated fat and tropical oils with healthy fat, such as nuts and peanut butter.”
Team Novo Nordisk, a global team made up of triathletes, runners and cyclists with Type 1 diabetes founded in 2006 teamed up to prove people with the disease can still participate in endurance sports.
This year from June 11-17 the 16 pro-riders participated in ‘Pedal for 7’, a seven-day UK tour, as they pass through various “United Kingdom towns covering 553 miles through the week,” according to Xpose.ie.
In the article “Going Long: Spring Endurance Sports and Diabetes" written by Matthew Butterman for the blog Diabetes Daily cited Dr. Rafael Castol who works with Team Novo Nordisk and recommended a blood glucose range of 120-180 mg/dL for the team.
“Cyclists on Team Novo Nordisk will often compete in races between 100-160 miles in length or 4-7 hours of duration. For these lengthy endurance efforts, Dr. Castol recommends that athletes eat a mixture of 80 percent of carbohydrate and 20 percent of protein during the first two hours of the race, and from 2-4 hours they will rely on energy bars, fruit, and electrolyte drinks,” said Butterman.
Edward Horton, a professor of medicine at Harvard Medical School and investigator at the Joslin Diabetes Center worked with both diabetic and non-diabetic endurance athletes while studying their glucose metabolism.
In an article for Outside Magazine written by Alex Hutchinson, Horton said the nature of serious endurance athletes, who are neither obese nor inactive, belies an often hidden health risk.
Dr. Peter Attia, a long-distance swimmer and cyclist, discovered in 2009 he had insulin resistance despite exercising three or four hours a day. Tim Noakes, a marathon runner and the author of “The Lore of Running,” developed pre-diabetes the same year.
Both had the same underlying cause to their diabetes, a carb-loaded diet.
According to Hutchinson’s article in Outside Magazine, researchers found that elite endurance athletes have insulin sensitivity that is roughly three times higher than healthy non-athletes, meaning they rapidly get the sugar they consume out of their bloodstream and into their muscles without having to produce excessive amounts of insulin.
Although endurance athletes are usually known to consume a high number of calories, Colberg-Ochs is conducting a clinical study in Scandinavia to “examine the effects of very low-carb eating on blood glucose levels in adults with type 1 diabetes.”
Colberg-Ochs surveyed over 275 active individuals with diabetes and found, surprisingly, a large number of athletes claimed to be following a very “low-carb dietary regimens.”
“Based on their responses, it appears entirely possible to undergo fat adaptation and exercise regularly — at least when engaging in endurance type training and events. These exercisers worry less about getting hypoglycemic during events as they have lower levels of insulin on board, but many others accomplished the same reduction in the risk of lows simply by not taking bolus insulin (doses specifically meant to be taken with meals) within a few hours of being active (even if eating more daily carbs).”
The active individuals reported they were consuming only 20 grams of carbs a day. Colberg-Ochs said on average an active individual consumes 2,000 calories per day and gets 15 percent of their calories from carbs. That equals 75 grams per day, which is much more than the 20-30 daily grams the athletes claim to be eating.
In order to determine how low-carb athletes with diabetes need to perform, Colberg-Ochs said it all depends on the sport and level of athlete.
“If you decide to try a low-carb diet, keep in mind that adapting to training with fewer daily carbs requires several weeks, so don’t just cut carbs for a few day and expect to feel good during any type of exercise,” Colberg-Ochs said.
Edith Noriega is a junior journalism student at Arizona State University.